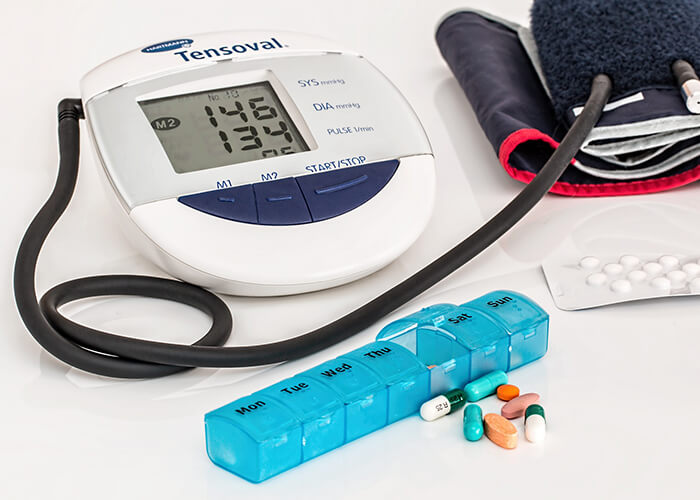
High Blood Pressure
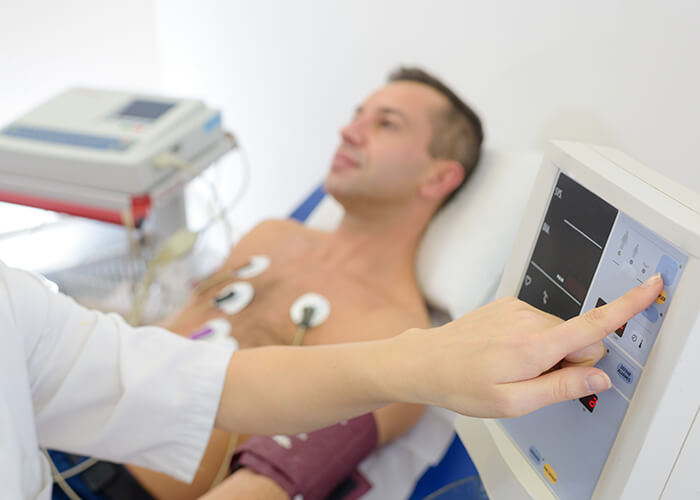
Diagnosis & therapy
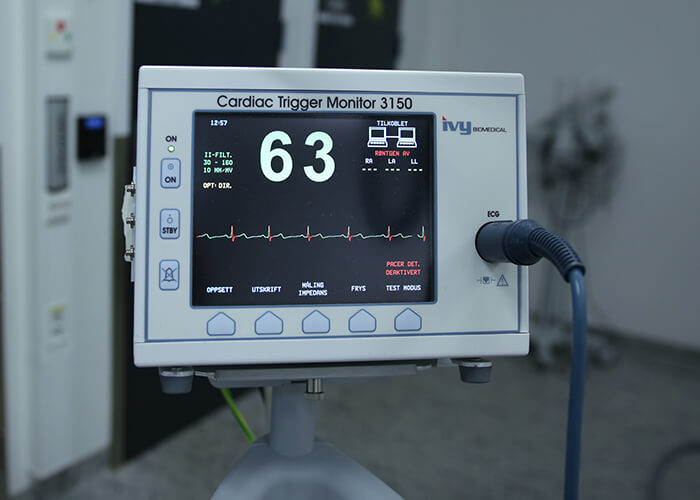
Blood pressure and heart rate change constantly and are also subject to sudden fluctuations. This is quite normal and also makes sense, because in this way the body can quickly adapt to changing exertion levels. For example, to be particularly capable of responding physically in an emergency, your pulse or blood pressure will need to increase within seconds. Slight variations in blood pressure (unstable blood pressure) are for this reason healthy and normal. One prerequisite for a diagnosis of high blood pressure is that the blood pressure be permanently elevated even while at rest.